Hemorrhoids are a common condition, but for some, they can become a recurring problem, leading to ongoing discomfort and frustration. If you’ve experienced hemorrhoids that come back frequently, you’re not alone.

What Are Recurring Hemorrhoids?
Recurring hemorrhoids refer to hemorrhoids that continue to flare up over time, despite treatment. Hemorrhoids themselves are swollen veins in the rectal or anal area, caused by increased pressure during bowel movements, prolonged sitting, or other factors. Once a person has experienced hemorrhoids, the chances of recurrence can increase, particularly if the underlying causes are not addressed.
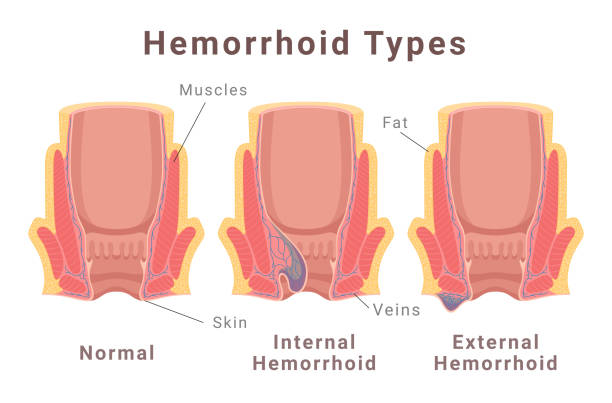
Common Causes of Recurring Hemorrhoids
There are several factors that contribute to the recurrence of hemorrhoids:
Chronic Constipation or Straining:
Constant straining during bowel movements puts pressure on the veins in the rectum, leading to hemorrhoids that can come back after treatment.
Diet Lacking in Fiber:
A low-fiber diet can cause hard stools, increasing the risk of constipation and hemorrhoids.
Prolonged Sitting:
Sitting for long periods, particularly on the toilet, can contribute to hemorrhoid development and recurrence.
Obesity and Lack of Physical Activity:
Being overweight or sedentary can increase pressure on the lower rectum, leading to recurring hemorrhoids.
Pregnancy:
Pregnancy increases pressure in the pelvic area, often causing hemorrhoids that can return after childbirth if lifestyle changes aren’t made.
Symptoms of Recurring Hemorrhoids
The symptoms of recurring hemorrhoids are similar to those experienced during an initial flare-up. These include:
- Itching, irritation, or pain around the anus
- Swelling or lumps near the anus
- Discomfort during bowel movements
- Ocassional bleeding, especially when straining

How Can one Prevent Hemorrhoids from Recurring?
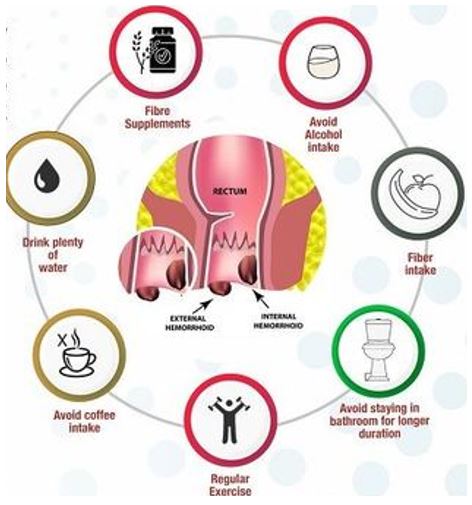
The good news is that recurring hemorrhoids can often be prevented with lifestyle adjustments. Here are some practical tips to help keep hemorrhoids from coming back:
Increase Fiber Intake:
A diet rich in fiber—from fruits, vegetables, legumes, and whole grains—helps soften stools and adds bulk, making bowel movements smoother and easier to pass. This reduces strain on the rectal veins, which is a key factor in preventing hemorrhoids. Aim to gradually increase your fiber intake to avoid bloating, and consider a fiber supplement if you’re not getting enough through food alone.
Stay Hydrated:
Drinking plenty of water throughout the day supports proper digestion and helps fiber do its job effectively. Adequate hydration keeps stools soft and prevents constipation, one of the leading causes of hemorrhoids. As a general guideline, try to drink enough fluids so your urine stays light in color.
Exercise Regularly:
Consistent physical activity stimulates bowel function and helps prevent constipation by encouraging regular movement in the digestive tract. Even moderate activities like walking, swimming, or yoga can improve circulation and reduce pressure on rectal veins, lowering the risk of flare-ups.
Avoid Straining:
Straining during bowel movements places excessive pressure on the veins in the rectal area, which can worsen or trigger hemorrhoids. Try to go as soon as you feel the urge, and avoid sitting on the toilet for extended periods. If needed, stool softeners or fiber supplements can make the process easier and more comfortable.
Limit Sitting Time:
Prolonged sitting—especially on hard surfaces or the toilet—can increase pressure on the lower rectum and contribute to hemorrhoid development. Take regular breaks to stand, stretch, or walk around, particularly if you have a desk job or sedentary routine.
Maintain a Healthy Weight:
Carrying excess weight, particularly around the abdomen, can increase pressure on the pelvic and rectal veins. Maintaining a healthy weight through balanced nutrition and regular exercise helps reduce this pressure and lowers the chances of hemorrhoids recurring over time.
Treatment Options for Recurring Hemorrhoids
If you experience recurring hemorrhoids, a variety of treatment options are available to manage them effectively.
Medical Treatments for Recurring Hemorrhoids
For more severe cases, especially if home treatments don’t provide relief, medical intervention may be necessary. Common treatments include:
- Rubber Band Ligation: A minimally invasive procedure where a small rubber band is placed around the base of the hemorrhoid, cutting off its blood supply and causing it to shrink.
- Transanal Hemorrhoidal Dearterialization: THD is a more advanced procedure that targets the blood vessels supplying the hemorrhoids.
When Should You See a Doctor?
While many hemorrhoid cases can be managed at home, recurring hemorrhoids that persist or cause severe discomfort should be evaluated by a doctor. Seek medical attention if:
- Hemorrhoids cause significant pain or bleeding
- Home remedies and over-the-counter treatments are not effective
- You experience hemorrhoids that protude or prolapse frequently
- You notice changes in your bowel habits that last for more than a few seconds
Recurring hemorrhoids can be a persistent issue, but with the right combination of lifestyle changes, home remedies, and medical treatments, they can be managed effectively. By focusing on prevention—through diet, exercise, and healthy bowel habits—you can significantly reduce the likelihood of hemorrhoids coming back.
If you’re struggling with recurring hemorrhoids, don’t hesitate to consult a healthcare provider for personalized advice and treatment options that will help you regain comfort and peace of mind.
-Disclaimer-
The information provided on this website is for educational and informational purposes only and is not intended as medical advice. Always consult with a qualified healthcare provider regarding any medical concerns, conditions, or treatment options. Individual results may vary. The information provided or services described are not intended to diagnose, treat, cure, or prevent any disease. Any medical or aesthetic procedure should be discussed thoroughly with a licensed professional before beginning treatment.

